
Features
Structural
Training
Trainer’s Corner: February 2010
In December’s column we looked at the unique challenges facing those responding to incidents of terrorism. In part 2 of our Olympics primer, we’ll focus on incidents involving multiple patients. Here are some examples of recent multiple-patient responses:
February 17, 2010
By Ed Brouwer
In December’s column we looked at the unique challenges facing those responding to incidents of terrorism. In part 2 of our Olympics primer, we’ll focus on incidents involving multiple patients. Here are some examples of recent multiple-patient responses:
- Whiteout conditions in the eastern part of Prince Edward Island on Dec. 19, 2008, led to a total of seven damaged vehicles and three people sent to hospital.
- A van carrying a high school boys’ basketball team home from a game was just five minutes from waiting parents on Jan. 12, 2008, when it fish-tailed on a slippery highway and slammed into a truck, killing seven players and an adult.
- John Pham, 10, of Mississauga, Ont., was killed on April 11, 2007, and 13 others were injured when their school bus collided with a tractor trailer during a field trip.
- Seven children suffered minor injuries when their bus crashed and caught fire during a January 2007 storm in Ottawa.
- Ten students were injured in September 2006 near Redvers, Sask., when a car, trying to pass a truck, collided with their bus.
- Eleven people were injured near Dafoe, Sask., in August 2006 when their bus left the road and rolled over.
- Five teenagers and their bus driver were treated in hospital for whiplash and cuts after their bus crashed into a tree near West Gore, N.S., in May 2006.
- Six children and three adults were injured in December 2005 near Cornwall, Ont., when their bus was broadsided by a minivan.
- Four children were slightly injured on November 2005 near Thorburn, N.S., after their bus swerved to avoid a rabbit.
- Eight children were slightly injured when their bus
- collided with a car near the village of Innerkip, Ont., in September 2005.
- Seven high school students were sent to hospital with minor injuries after their bus drove off the road in April 2005 near the town of Gaspereau, N.S.
- Five students from Abbotsford, B.C., went to hospital for treatment after two school buses and a cargo van got into an accident in February 2005.
As you can see from these news headlines, there is a distinct possibility that you may be called to a multi-patient incident. The initial actions of the first-arriving officer have to be directed toward scene size-up, requesting appropriate resources and initial organization of the scene. It boils down to three questions: What do I have? What action will I take? What resources do I need?
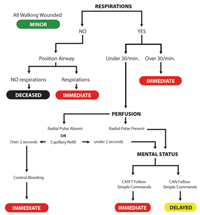 |
|
| The START (Simple Triage And Rapid Treatment) system was developed in 1983 by staff of Hoag Hospital and the Newport Beach Fire Department in California and is well suited to multi-patient incidents. Click here to view larger.. |
Command should rapidly survey the scene to identify any hazards or safety concerns and establish a safe zone in which crews can operate.
Triage should be started early, especially when the number of patients and/or the severity of their injuries exceeds the capabilities of the on-scene personnel to provide effective extrication, treatment and transportation. Once triage is complete, a triage report should be radioed to dispatch.
The IC needs to quickly determine the most effective means to treat patients. In incidents with few patients, it may be more effective to treat patients in place. At incidents with a greater number of patients, a treatment area should be established.
Once the triage group has identified and sorted all patients, command should be contacted and given a triage report. This includes the number of patients and their conditions. A typical triage report may sound like this: “Command – triage.” Go ahead triage. “Triage has been completed. We have two immediates, three delayed and four minor.”
Command uses the triage report to call for additional resources or to scale back the response, and relays this information to dispatch.
A triage report becomes the triage benchmark, similar to the way an “all clear” signifies the completion of a search and rescue at a fire incident.
This means that all patients have been triaged and are ready for transfer to treatment or transportation based on the severity of injury.
Some incidents may require patients to be extricated from the scene to the patient treatment area before triage has been performed. This may be due to safety considerations due to the nature of the incident.
In some situations, patients are discovered and identified as the incident proceeds. The officer should relay a triage update to the IC.
Multiple-patient incidents may be rare but firefighters must be ready to effectively deal with them.
■ The START system
START (Simple Triage And Rapid Treatment) was developed in 1983 by staff of Hoag Hospital and the Newport Beach Fire Department in California (www.start-triage.com)
to quickly identify and sort patients during a multiple patient incident. START quickly distinguishes between critically injured victims and the less-severely injured.
Following a specific algorithm, a first responder quickly assesses airway, breathing, circulation and LOC (level of consciousness) to categorize a patient’s condition. With START, a triage team of two can assess an average of one patient every 30 seconds.
At an incident with 40 patients, two triage teams will take approximately 10 minutes to accurately triage patients using the START process. The only treatment rendered by the triage team is to open a patient’s airway by head/tilt neck lift or by insertion of an OPA (oropharyngeal airway), or to apply direct pressure to stop an obvious bleed or by elevating the extremities.
START was used successfully during the World Trade Center and Oklahoma City bombings. Several countries including France, Saudi Arabia and Israel have adopted the START program.
The three items that are checked when using START are respiration, perfusion (pulse) and mental status (RPM).
There are four classifications under which patients can be placed: immediate (red); delayed (yellow); minor (green); and dead/dying (black).
Immediate (red) are patients whose RPM is altered.
Patients unable to follow instructions to evacuate the scene, but whose RPM is intact are categorized delayed (yellow). This is the most common category. It also includes patients who have a significant mechanism of injury, but whose RPM is intact.
Minor (green) patients are able to leave the impact area on the instruction of EMS personnel. They are the walking wounded and should be tagged later.
The dead/dying (black) are those who cannot breathe after the airway is opened and/or those who are mortally wounded. These patients will probably die despite the best resuscitation efforts. It is often a difficult decision to leave a dying patient, especially a child. But remember – resources are often wasted on unsalvageable victims.
The three medical treatments rendered when performing START triage are: open an airway or insert an OPA; stop any visible bleeding; elevate the extremities for shock.
■ Triage priorities
Your initial goal during triage is to find immediate (red) patients. Your efforts should focus on locating all immediate patients, getting them treated and transporting them as soon as possible. Once immediate patients have been treated and transported, reassess all delayed patients and upgrade any to “immediate-by-mechanism,” depending on their injuries, age and medical history.
When performing triage, regardless of incident size, don’t become distracted; move quickly and focus your attention on immediate patients. Those are the real lives you’ll save. The goal is to stay focused on red.
Start where you stand and walk either clockwise or counter clockwise. As you approach, identify the uninjured or walking wounded. Move them out of danger or use them to control bleeding or to maintain an airway. Then, proceed to the victims who cannot move.
■ Triage assessment
Step 1. Respiration (Breathing)
- A. If none, open airway. If still no breathing, tag as deceased.
- B. If the breathing rate is greater than 30 per minute (meaning the patient might be in shock) or less than 10 beats per minute, tag the patient immediate.
- C. Respiration/breathing between 10 and 30 per minute, go to Step 2.
Step 2. Perfusion Check (radial pulse) or use a capillary blanch test
- A. Squeeze nail bed, palm of hand or pad of finger.
- B. If colour regains in greater than two seconds, tag immediate.
- C. If the colour returns in less than two seconds go to Step 3 – Mental Status.
- D. In poor lighting, attempt to find the radial pulse. If radial pulse is present proceed to Step 3.
Step 3. Mental Status
- A. Altered mental status is the inability to follow simple commands. If the patient is unable to follow simple commands, tag the patient immediate.
- B. If patient is able to follow simple commands, tag delayed.
- C. Example of simple commands: “Squeeze my hands”, “Open and close your eyes”.
■ Rapid treatment
Ventilation
A. Open airway, clear obstructions or blood from airway.
B. Use pocket mask.
■ Circulation
A. Apply a quick bandage; “walking wounding” can assist.
B. Raise legs to return blood to the heart.
Note: If victim is unconscious, mark as immediate.
We need to prepare for the worst if we expect to do our best. I have more information regarding START; dealing with more than 25 or more than 40 casualties, as well as a copy of the START triage tags. Drop me a line at ed@thefire.ca.
Until next time, stay safe and be sure to train like their lives depend on it, because they do.
Ed Brouwer is the chief instructor for Canwest Fire in Osoyoos, B.C., and the training officer for West Boundary Highway Rescue. The 19-year veteran of the fire service is also a fire warden with the B.C. Ministry of Forests, a wildland interface fire suppression instructor/evaluator and a fire-service chaplain. Contact Ed at ed@thefire.ca
Print this page